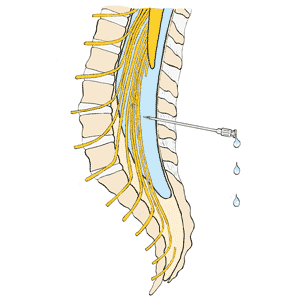
Description of the test
The brain and spinal cord make up the central nervous system, which allows us to think, move, see, hear, touch, taste, and speak. Surrounding the brain and spinal cord is a fluid called cerebrospinal fluid (CSF) that cushions and nourishes these areas. The spinal tap test provides information about this fluid and the areas it surrounds.
The test also measures the pressure of this fluid. Changes in the contents or pressure of this fluid may indicate a health problem in the brain or spinal cord.
Testing of CSF takes place in a hospital or at your doctor's office. Your doctor or another health care professional will remove the fluid with a needle.
How often should the test be performed?
Your doctor will decide when and how frequently this test is required to provide medical information.
Why is this test performed?
A spinal tap is used when doctors need information to determine if someone has a serious infection, such as meningitis, a central nervous system disorder (e.g., multiple sclerosis, Guillain-Barre syndrome, bleeding) or cancer.
Are there any risks and precautions?
Although a spinal tap is generally considered safe, it does have some risk of side effects or complications. These include:
- nerve or brain damage (uncommon)
- bleeding in the spinal column
- damage to the spinal column
- infection
- allergic reactions to the anesthesia (the medication used to numb the area where the needle is inserted)
- lower back pain
Up to 25% of people will develop a headache after the test. Headache tends to resolve on its own without any treatment.
However, a headache lasting more than 1 or 2 days after the test may be a sign that CSF is leaking out of your spinal canal. See your doctor immediately if this happens. This type of leak may close on its own with rest, or with an injection of your own blood that will seal the leaking area.
Other problems related to changes in pressure inside the spinal canal and brain may occur.
If you are concerned about any symptoms following this test, speak to your doctor. Take the time to be sure you understand all the risks of complications and side effects as well as any precautions you or your doctor can take to avoid them. Be sure your doctor understands all your concerns.
What happens during the test?
Before the test starts, you may be asked to empty your bladder. Then you will be asked to undress either partially or fully and put on a hospital gown. You will lie down (on your side) on an examination table or hospital bed and draw your knees up to your chest. Your doctor may ask you to take another position; however, this is the most common position for the test.
The doctor looks at your spinal column, then marks where a needle will be inserted into your spine. Cleaning the area with an antiseptic solution prepares the area and reduces the number of bacteria that may cause infection.
A local anesthetic is used to freeze the area before another needle is inserted for the test. The doctor inserts the needle where CSF is likely accessible. If the doctor is successful, CSF will leak out into the needle. If no CSF comes out, the doctor must reposition the needle. You may feel stinging or discomfort during this process. It is important to stay completely still while the needle is being inserted.
Your doctor may take pressure readings, one when the spinal canal is first punctured, and another before the needle is removed. The readings are called the opening and closing pressures, respectively.
The test takes approximately 30 to 45 minutes.
How should I prepare for this test?
Before having this test, discuss the advantages, disadvantages, long-term risks, and consequences associated with the test with your doctor. Be sure you fully understand what will happen and are comfortable with your doctor's answers to your questions.
Tell your doctor or prescriber about all prescription, over-the-counter (non-prescription), and herbal medications you are taking. Also tell them about any medication allergies and medical conditions that you may have. Tell your doctor before the test if you are allergic to anesthetic or if you are or may be pregnant.
Some medications and medical conditions may affect the test. Blood disorders or medications that decrease the ability of the blood to clot (e.g., blood thinners) may increase the chances of bleeding. Your doctor may order some blood tests to see if you have any bleeding disorders. Your doctor may also want you to have a computed tomography (CT) scan before having a lumbar puncture to make sure there is no swelling around or in your brain.
Ask your doctor or pharmacist whether you need to stop taking any of your medications before the procedure.
If you are planning to return home on the day of the test (i.e., if you have not been admitted to the hospital), you should arrange for someone to drive you home.
What can I expect after the test?
After testing, you will probably be asked to lie in bed for several hours. To replace any fluid removed, you may need to drink extra liquids. Follow your doctor's instructions closely after the test to reduce any risk of complications.
You can usually return to your normal activities 24 hours after the test is completed, but check with your doctor for instructions.
You may also notice fatigue, a mild backache, or difficulty sleeping for a day or two after the test.
Results
A neurologist usually interprets the test results. Some test results are ready immediately after the test. Others take a few days or several weeks to return from laboratory analysis.
The laboratory looks at various characteristics of the CSF. Your doctor considers the color, pressure, protein levels, glucose levels, cell counts (e.g., red and white blood cell counts), and other results from the test to help with your diagnosis.
Generally, problems with pressure of the CSF indicate swelling, infection (e.g., meningitis), or bleeding in the brain. High protein levels may be caused by a variety of factors, including blood in the CSF, a tumour, an infection, inflammation due to multiple sclerosis, or nerve damage (e.g., Guillain-Barré Syndrome).
Glucose levels are also measured. High glucose levels are associated with diabetes, while low glucose levels are often caused by bacterial infections. High white blood cells usually mean there is an infection.
The results will help your doctor decide on a diagnosis, treatment options, and whether other tests may be needed.
All material copyright MediResource Inc. 1996 – 2024. Terms and conditions of use. The contents herein are for informational purposes only. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Source: www.medbroadcast.com/procedure/getprocedure/Spinal-Tap