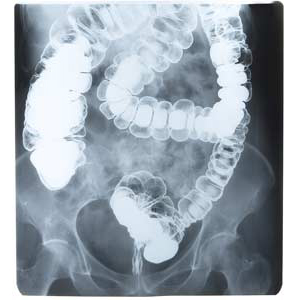
Description of the test
A barium enema is a test in which X-ray pictures are taken of the colon. It involves placing a white liquid called barium into the rectum and colon. Barium is a contrast material that helps to enhance X-ray pictures for clearer images. This test is done to visualize the anatomy of the colon and to diagnose conditions such as inflammatory bowel disease and colon cancer.
How often should the test be performed?
A barium enema may be part of a screening program for colon cancer, especially for people who cannot have a colonoscopy. Your doctor may also recommend a barium enema at any time to help determine the cause of symptoms (e.g., diarrhea, abdominal pain) you are experiencing.
Why is this test performed?
Barium enemas are used to diagnose colon and rectal cancers as well as inflammatory diseases. They are used to detect polyps (benign growths on the lining of the colon or rectum), diverticula (out-pouchings of the colon), and structural changes of the colon.
If you experience a change in your bowel habits, your doctor may order a barium enema to help evaluate your symptoms. For example, a barium enema may be necessary to explain symptoms such as diarrhea, blood in the stool, or abdominal pain.
Are there any risks and precautions?
The barium enema does involve some radiation exposure. Exposure to radiation is minimized by standardizing the techniques used by the radiologist and radiation technologist.
Notify the radiology staff and your doctor ordering the test if you are allergic to barium or latex, have recently had a barium swallow procedure, or are or may be pregnant. Radiation exposure may be harmful to the fetus.
Occasionally, the barium can harden in the colon and cause severe constipation or obstruction. This is a rare complication and can be prevented by drinking extra fluids after the test and taking a laxative or enema if necessary. Rarely, barium granulomas (inflamed areas of the colon) can form.
Very rarely, the colon may be perforated (torn) during a barium enema and the contents of the colon may spill into the intestinal cavity. This complication can be treated with surgery and antibiotics.
If you have a perforation (tear) in the intestine, severe ulcerative colitis, or toxic megacolon (a life-threatening condition where the colon dilates or widens quickly), you should not have a barium enema.
What happens during the test?
You will be asked to change into hospital gown and to lie on an X-ray table.
An X-ray may be taken before barium is inserted to ensure that the colon and rectum are cleaned out enough. A well-lubricated rectal tube will be inserted into the rectum to administer the barium. Throughout the examination, you will be asked to tightly contract your anal muscles to ensure that the rectal tube stays in place and to prevent the barium from leaking. You may feel fullness, discomfort in your abdomen (cramping), and an urge to defecate while the barium is in place. This is normal. Take slow deep breaths to help ease the discomfort.
After the barium fills the colon, air may be slowly injected to inflate the colon. The radiologist then takes multiple images of the colon with a type of X-ray called fluoroscopy, which allows images to be immediately visible on a screen. You will be required to roll into several different positions (on your sides, your back, and your front) during the examination. A technologist will be available to help you if you have trouble moving around. The X-ray table may move around underneath you and may be tilted so that you are in an almost upright position. The radiologist or technologist will warn you before this happens. You will be closely monitored to make sure you do not fall from the table. The examination can take between 30 and 45 minutes, depending on what the doctor is looking for.
After the images have been taken, the rectal tube will be removed along with most of the barium and you will be able to expel the remaining barium from the bowel. Some additional pictures may be taken after expelling the barium.
How should I prepare for this test?
A clear liquid diet, laxatives, and possibly cleansing enemas are required to clear the colon, usually 1 to 3 days before the test. Drinking large amounts of water 12 hours before the test is encouraged, unless your health professional tells you otherwise. This preparation is important as any fecal material remaining inside the colon will interfere with the clarity of the images. Follow the instructions provided to you.
Tell your doctor or prescriber about all prescription, over-the-counter (non-prescription), and herbal medications that you are taking. Also tell them about any medication allergies and medical conditions that you may have. Ask your doctor or pharmacist whether you need to stop taking any of your medications before the test. Most medications can be taken as usual with a small amount of water, but check with your doctor first.
Arrange for someone to drive you home from the hospital or clinic.
What can I expect after the test?
Drink plenty of fluids after the test and in the following few days, to clear the barium from the colon and counteract the constipating effects of the barium. You may have light-coloured stools for up to 3 days after the test. You may also feel very tired after the test, so get plenty of rest.
Results
The radiologist will look at the X-rays and will send a report to your doctor. Your doctor can then share the results with you. Test results are usually available after a few days.
All material copyright MediResource Inc. 1996 – 2024. Terms and conditions of use. The contents herein are for informational purposes only. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Source: www.medbroadcast.com/procedure/getprocedure/Barium-Enema