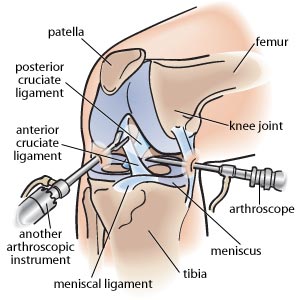
Description of the test
Arthroscopy is a test used to examine joints and surrounding tissues, and to repair joint problems (including complications related to arthritis or sports injuries). A surgeon inserts a tube called an arthroscope into the joint through small incisions in the skin. A small camera on the tube with a light attachment allows the surgeon to display images of the joint on a video screen. Later, the surgeon may insert other tools through the arthroscope to repair the joint.
The test takes place in a hospital or clinic. Orthopedic surgeons often perform this test. The use of either general or local anesthesia depends on which joint is being tested.
How often should the test be performed?
Your doctor will decide when and how frequently this test is required.
Why is this test performed?
An arthroscopy is performed to diagnose joint problems. These joints include wrists, shoulders, knees, ankles, elbows, or hips. It is also performed to surgically repair a joint problem.
If you require arthroscopy, it is likely because you have:
- symptoms related to certain bone conditions (e.g., arthritis, osteoporosis, rheumatoid arthritis, bone spurs)
- an inflammation of a joint
- damaged ligaments or tendons, or cartilage
- an infection of a joint
- pain in joints or bones that has not been diagnosed
During an arthroscopy, a doctor can also remove samples (a biopsy) of the bone and joint for microscopic examination in a lab. An arthroscopy can also help doctors monitor whether a specific medications or treatments are working over time.
Are there any risks and precautions?
Arthroscopy is a relatively safe procedure and complications are rare. These complications may include bleeding, infection, blood clots, damage to surrounding muscles and ligaments, nerve or blood vessel damage, or a reaction to the general anesthesia.
If you experience fever, bleeding, or drainage from the incision, this may indicate infection - call your doctor. Additionally, call your doctor if you feel numbness, tingling, or pain at the test site.
If you are concerned about any symptoms following this procedure, speak to your doctor.
Take the time to be sure you understand all the risks of complications, side effects, as well as any precautions you or your doctor can take to avoid them. Be sure your doctor understands all your concerns.
What happens during the test?
You will receive a local, general, or regional anesthesia for this procedure. General anesthesia will put you completely to sleep and is given through an intravenous (IV) needle. Regional and local anesthesia numb the specific area for the test while you are still awake. After the anesthetic is given, you will not feel any pain during the procedure, although with local anesthesia you may still feel pressure.
You will be asked to remove your clothes and accessories and dress in a hospital gown. The skin around your joint may need to be shaved.
The doctor places a band around the area to restrict blood flow to the joint before disinfecting the area. The surgeon makes a small incision in the skin around the joint and inserts the arthroscope. The camera on the arthroscope displays the image of the joint on the video screen, making it possible for the doctor to identify and repair problems or to take samples. Bending and moving the joint to various positions may be necessary throughout the test. Other small incisions may be made around the joint in order to insert surgical tools if needed. The instruments may be used to cut, grind, or remove damaged tissue.
The doctor will irrigate the joint with solution throughout the procedure to clean out the joint. The incision will be stitched and covered with sterile bandages. You may need to use crutches, a sling, or a splint to help the affected area heal. The procedure takes about 30 minutes to 2 hours.
How should I prepare for this test?
Before having this procedure, discuss the advantages, disadvantages, or long-term risks and consequences associated with the procedure with your doctor. Be sure you fully understand what will happen and are comfortable with your doctor's answers to your questions.
Your doctor needs to know if you:
- are or may be pregnant
- are taking any medications, and what they are
- are allergic to any medications
- are allergic to anesthesia
- have an infection near the affected area
Since you will be receiving an anesthetic and possibly pain medications, arrange for someone to drive you home after the procedure.
Do not eat for 8 hours before the procedure. You may continue to drink clear liquids until 2 hours before the procedure. If your doctor has recommended different times, follow the timing recommended by your doctor.
Tell your doctor or prescriber about all prescription, over-the-counter (non-prescription), and herbal medications that you are taking. Also tell them about any medication allergies and medical conditions that you may have.
Ask your doctor or pharmacist whether you need to stop taking any of your medications before the test.
What can I expect after the test?
You will likely feel some or all of these normal side effects after the test:
- pain
- swelling for several days
- bruising
- tenderness of the area
To prevent infection, it is important to keep your bandages clean and dry. Take pain medication and apply ice as instructed by your doctor. Your doctor may also prescribe an antibiotic in order to prevent infection. You may be given exercises to do so that you can strengthen the muscle around the joint. Most people will need to rest for at least one week before returning to work. The length of your recovery period depends on your specific situation.
Results
Your doctor reviews the test and images taken during the test to assess your joint. Your doctor may discuss the results with you immediately following the test.
All material copyright MediResource Inc. 1996 – 2024. Terms and conditions of use. The contents herein are for informational purposes only. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Source: www.medbroadcast.com/procedure/getprocedure/Arthroscopy