Description of the procedure
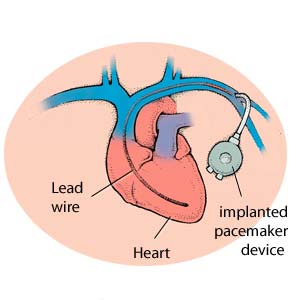
A pacemaker is a small battery-powered electronic device that is surgically implanted, usually in your chest, to monitor and regulate abnormal heart rate and rhythm (arrhythmia).
A pacemaker consists of a pulse generator and leads. The generator produces electrical signals and the leads (insulated wires) transmit the signals to the heart.
When should this procedure be performed?
Your doctor will recommend this procedure when required.
Why is this procedure performed?
When the heart no longer beats with a normal rhythm, a doctor may suggest a pacemaker. An abnormal heart rhythm may happen for a number of reasons:
- aging
- damage to the heart muscle from a heart attack
- problems with the heart's electrical system
- use of certain medications (e.g., beta-blockers)
- imbalance of minerals called electrolytes in your body (e.g., sodium, potassium, calcium)
- certain medical conditions (e.g., diabetes, hyperthyroidism)
An abnormal heart rhythm can have a major impact on a person's daily activities. Household chores, exercise, and other normal activities can lead to dizziness, fainting, and fatigue because of the poor blood and oxygen supply to the body. Palpitations can also occur.
Are there any risks and precautions?
Certain risks are common to all surgery and every time a local or regional anesthetic is used. These risks depend on many factors including the type of surgery and your own medical condition. The possible, but very rare, side effects include: side effects of the anesthetic, breathing problems, infection, and bleeding.
Although pacemaker surgery is generally considered safe, it does have some risk of side effects or complications. These include:
- blood clots
- damage to the blood vessel and heart muscle
- stroke
- heart attack
- puncture of the lung and collapsed lung
- swelling or bruising at the site where the generator was implanted
- allergic reaction to the sedative or anesthetic
- bleeding
- infection
If you experience these side effects or complications, contact your doctor immediately.
If you are concerned about any symptoms following this procedure, speak to your doctor. Take the time to be sure you understand all the risks of complications and side effects as well as any precautions you or your doctor can take to avoid them. Be sure your doctor understands all your concerns.
What happens during the procedure?
The procedure is usually performed under local anesthesia by a surgeon or cardiologist. You will also be given a sedative to help you relax. This procedure is done with the help of an X-ray machine.
- Through an opening made below the collarbone, insulated wires (also known as leads) are inserted into a large vein and attached to the chambers on the right side of the heart. For some heart conditions, the wires are attached to the right and left sides of the heart.
- With one end of the wires attached to the heart, the other ends are connected to the pacemaker. A pocket is made under the skin or under the muscle in the upper chest, and the pacemaker is placed in this pocket.
- The opening is then stitched closed.
The procedure typically takes 1 to 2 hours.
How should I prepare for this procedure?
Do not eat for 8 hours before the procedure. You may be able to drink clear liquids until 2 hours before the procedure. If your doctor has recommended different times, follow the timing recommended by your doctor.
Tell your doctor or prescriber about all prescription, over-the-counter (non-prescription), and herbal medications that you are taking. Also tell them about any medication allergies and medical conditions that you may have. Arrange for someone to drive you home from the hospital.
Ask your doctor or pharmacist whether you need to stop taking any of your medications before the procedure.
Follow any additional instructions from your doctor.
What can I expect after the procedure?
Some people are sent home the same day, but most remain in the hospital for 1 to 2 days. While there, the doctors will check the pacemaker using a heart monitor and adjust the settings if necessary.
There are certain precautions you must take to keep your pacemaker working properly. For the first few days, do not raise your arms above your head. If you do, the wire leads that attach to the heart may move and the pacemaker will not work. Your doctor may also advise you to avoid heavy lifting and strenuous exercise for a few weeks.
Once you leave the hospital, it is important to:
- Avoid standing too close to certain mechanical equipment as they may interfere with the electrical signals from the pacemaker (e.g., welding equipment, high-power generators). Discuss what is considered a safe distance with your doctor.
- Make sure security personnel at airports or other areas know about the pacemaker, since it may set off these security systems.
- Tell your doctors or other health care professionals that you have a pacemaker in order to avoid problems with certain diagnostic equipment (e.g., magnetic resonance imaging [MRI] machines) and other procedures
Although cell phones are not likely to pose a significant health risk if you have a pacemaker, experts recommend the following precautions while using a cell phone:
- hold your cell phone at least 6 inches away from your pacemaker unit
- if your cell phone is turned on, do not put your cell phone in a shirt pocket over your pacemaker
- hold your cell phone to the ear on the opposite side of your pacemaker
You should follow-up with your doctor from time to time to check that your pacemaker is working properly. Pacemaker batteries generally last on average 5 to 10 years. Your doctor will change the batteries when it is needed. The leads may be replaced at the same time, if it is needed. Your doctor may be able to check your pacemaker over the telephone if your pacemaker has this feature.
Results
When properly implanted and functioning normally, the pacemaker will prevent your heart from beating irregularly.
All material copyright MediResource Inc. 1996 – 2024. Terms and conditions of use. The contents herein are for informational purposes only. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Source: www.medbroadcast.com/procedure/getprocedure/Pacemaker-Surgery