Description of the procedure
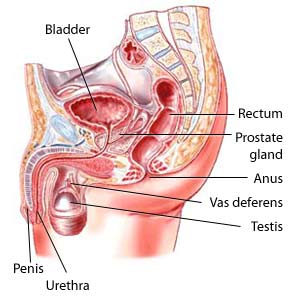
Radical prostatectomy is a surgical procedure to remove the prostate gland and some of the tissue around it. Radical prostatectomy is used to treat prostate cancer. An urologist performs this procedure in a hospital or clinic.
When should this procedure be performed?
Your doctor will recommend this procedure when required.
Why is this procedure performed?
The procedure is performed to treat prostate cancer. It is usually used when prostate cancer has not yet spread through the body and the man is otherwise in good health.
Are there any risks and precautions?
Certain risks are common to all surgery and anesthesia. These risks depend on many factors, including the type of surgery and your own medical condition. The possible, but very rare, side effects include reactions to the anesthesia, breathing problems, infection, bleeding, scarring, and death.
Although radical prostatectomy is generally considered safe, it does have some risk of side effects or complications. These include:
- lack of bladder control (also called urinary incontinence)
- decreased ability to hold your urine flow with increased pressure, such as when you sneeze, cough, or laugh (also called stress incontinence)
- loss of control of bowel movements (also called fecal incontinence)
- erectile dysfunction (problems getting or keeping an erection) due to nerve damage
- damage to nearby organs (such as the rectum)
If you are concerned about any symptoms following this procedure, speak to your doctor. Take the time to be sure you understand all the risks of complications and side effects as well as any precautions you or your doctor can take to avoid them. Be sure your doctor understands all your concerns.
What happens during the procedure?
This procedure is usually done with general anesthesia so you won't be awake. After the anesthesia is given, the doctor makes an incision from the top of the pubic bone to the navel. Some men may have the surgery performed laparoscopically (a few small incisions are made in the abdomen and a thin tube with a camera on the end allows the surgeon to see inside the abdomen). For some surgeries, the surgeon may use robotic arms in order to produce more accurate and precise movements.
Other instruments are inserted into the small incisions to perform the surgery. The prostate gland and surrounding tissue (seminal vesicles and part of the urethra) are removed. Sometimes, a small sample of tissue from the lymph nodes in the region is taken and checked for cancer before removing the prostate. If the lymph nodes have no cancer, then the prostate gland is removed.
In some situations, the surgeon may be able to save the nerves around the prostate to reduce the risk of the man being unable to have erections after the surgery. Because the urethra (the tube through which urine passes out of the body) is cut during the procedure, it must later be attached directly to the bladder.
Another less common approach for surgery is to make an incision between the anus and the scrotum, an area called the perineum. There is less bleeding with this approach, but there is a higher risk of rectal injury. As well, if any lymph nodes need to be removed, a second incision will be necessary.
How should I prepare for this procedure?
Before having this procedure, discuss the advantages, disadvantages, long-term risks, and consequences associated with the procedure with your doctor. Be sure you fully understand what will happen and are comfortable with your doctor's answers to your questions.
You may need blood tests several days or weeks before the surgery. Your doctor may also order a complete physical exam. To clear your colon before the procedure, your doctor may ask you to take a laxative the night before or use an enema the morning you go to the hospital.
Recovery time is often faster for people who exercise regularly. You can speed up the healing process by not smoking and losing weight, if necessary, before the procedure. Your doctor may also recommend that you do Kegel exercises to strengthen your pelvic muscles to help with recovery.
Tell your doctor about all prescription, over-the-counter (non-prescription), dietary supplements, and herbal medications that you are taking. Also tell them about any medication allergies and medical conditions that you may have.
Do not eat or drink anything after midnight the night before your surgery. . If your doctor has recommended different times, follow the timing recommended by your doctor.
Tell your doctor about all prescription, over-the-counter (non-prescription), and herbal medications that you are taking. Also tell them about any medication allergies and medical conditions that you may have.
Ask your doctor or pharmacist whether you need to stop taking any of your medications before the procedure.
Arrange for someone to drive you home from the hospital.
What can I expect after the procedure?
The surgery will take 2 to 4 hours. Staying at the hospital for 1 to 4 days after the procedure is normal. Your hospital stay may be shorter if you had laparoscopic or robot-assisted surgery. Pain medication will help you if you are uncomfortable or in any pain.
When you wake up from the surgery, you will probably have a catheter in your penis to drain urine from the bladder. Having the catheter is normal; however, it may be uncomfortable because it may make you feel as though you need to urinate. The catheter usually remains in place for about 1 to 3 weeks after you return home from the surgery.
Over time (usually 3 to 6 months), most men regain their bladder control through the use of Kegel exercises. These exercises help build the muscles on the pelvic floor that make it possible to control urination. Your doctor will recommend that you avoid strenuous exercise and heaving lifting for about 4 to 6 weeks after the surgery.
It generally takes men 4 to 6 weeks to recover from the surgery.
Results
Your doctor will usually wait 6 to 8 weeks after the surgery before testing your prostate specific antigen (PSA) levels (a prostate cancer screening test). Ask your doctor how often this test should be repeated for you.
Most, if not all, men notice a loss in their ability to get or keep erections. This is normal and may go away depending on your age, overall health before the procedure, and type and extent of surgery. Also, if no nerves were damaged during the procedure, you are less likely to experience problems related to sexual function.
Talk to your doctor about treatment options and what to expect.
All material copyright MediResource Inc. 1996 – 2024. Terms and conditions of use. The contents herein are for informational purposes only. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Source: www.medbroadcast.com/procedure/getprocedure/Radical-Prostatectomy