Description of the procedure
A mastectomy is the surgical removal of all breast tissue from one or more breasts. Mastectomies are performed by surgeons in a hospital operating room and are done under general anesthesia to treat and prevent breast cancer.
Not all women with breast cancer require a mastectomy. Breast-conserving surgery (or lumpectomy, where only the tumour is removed from the breast) combined with radiation and chemotherapy is another treatment option for many women with breast cancer.
Discuss these options with your doctor.
When should this procedure be performed?
Doctors perform this procedure as required to treat or prevent breast cancer. The procedure is permanent. Be sure you are comfortable with the procedure and how it will impact your life. Ask your doctor or health care professional any questions and concerns you have, and discuss with your partner before the procedure is performed.
Why is this procedure performed?
Mastectomies may be performed to prevent breast cancer in certain high-risk people. There are a number of situations where a mastectomy may be the most appropriate treatment option for breast cancer, including:
- several cancerous tumours present in different areas of the breast
- pregnancy, since radiation and chemotherapy can harm the fetus
- certain medical conditions where radiation therapy may not be tolerated
- a strong family history of breast cancer
- a genetic abnormality that increases your risk of the breast cancer returning
- breast cancer that is widespread and makes up a large portion of the breast
- previous radiation therapy to the breast area
- circumstances (personal, financial, or geographic) that make it undesirable or difficult to undergo radiation therapy
- presence of cancer despite previous lumpectomy
The decision to have a mastectomy is one that should be made after careful discussion with your doctor. Important determining factors include the size of the tumour and whether the cancer has spread to other parts of the body, and if so, where it has spread.
Are there any risks and precautions?
Certain risks are common to all surgery and every time a general anesthetic is used. These include side effects of the anesthetic, breathing problems, infection, bleeding, and death.
Although mastectomy is generally considered safe, it does have some risk of side effects or complications. The most common side effects or complications are:
- nerve damage resulting in muscle weakness
- numbness, tingling, and skin sensitivity
- infection
- scar formation
- shoulder pain
- lymphedema, which is swelling of the arm resulting from poor lymph fluid drainage due to lymph node removal; lymphedema can be a chronic condition that requires ongoing treatment
- hematoma (buildup of blood where the surgery was done)
- chronic pain
If you are concerned about any symptoms following this procedure, speak to your doctor. Take the time to be sure you understand all the risks of complications and side effects as well as any precautions you or your doctor can take to avoid them. Be sure your doctor understands all your concerns.
What happens during the procedure?
Several types of mastectomy are available to those who have breast cancer. The type of mastectomy a person decides to have performed depends on many factors such as the location, size, and type of cancer. The different types of mastectomies are:
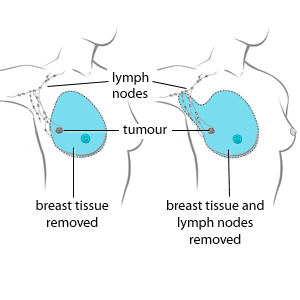
- simple or total mastectomy: Breast tissue, nipple, and areola (dark-coloured skin around the nipple) are removed, but not the underlying chest muscle or lymph nodes under the arm, although lymph node biopsy may be performed.
- modified radical mastectomy: Breast tissue, nipple, areola, and most or all of the lymph nodes under the arm are removed, and sometimes part of the underlying chest muscle.
- radical mastectomy: Breast tissue, nipple, areola, lymph nodes under the arm, and underlying chest muscle are removed. This procedure is almost never performed in modern surgical practice.
- skin-sparing mastectomy: Breast tissue, nipple, areola are removed but not the breast skin. Mastectomy is immediately followed by breast reconstruction surgery.
- nipple-sparing mastectomy: Only breast tissue is removed and not the skin, nipple, areola, chest wall muscles, and lymph nodes. Breast reconstruction is performed immediately after the mastectomy.
Just before the surgery, an intravenous (IV) line is placed in your arm so that your doctors can give you fluids and medication during surgery. An anesthesiologist first puts you to sleep using a general anesthetic that is given intravenously or inhaled. The surgeon then makes an incision in the breast and removes the necessary tissue depending on the type of mastectomy. After all the necessary tissue is removed, the incision is closed. Sometimes, breast reconstruction is performed right after the mastectomy.
Small plastic tubes may be left in place to allow fluid to drain. Your doctor will determine when these tubes are removed, usually 1 to 2 weeks later.
Following the procedure, you are sent to a recovery area to be monitored for any complications.
Normally the procedure takes 1 to 3 hours. It will require more time if you are having both breasts removed, or if breast reconstruction is part of the procedure.
How should I prepare for this procedure?
Before having this procedure, discuss the advantages, disadvantages, long-term risks, and consequences associated with the procedure with your doctor. Be sure you fully understand what will happen and are comfortable with your doctor's answers to your questions.
Your complete medical history is documented and an examination of the breast takes place before the procedure. Your surgeon will review your test results and may request other tests before the procedure. Talk to your doctor about reconstructive breast surgery. Some women have this at the same time as their mastectomy, while others have reconstructive surgery at a later date.
Tell your doctor about all prescription, over-the-counter (non-prescription), and herbal medications that you are taking. Also tell them about any medication allergies and medical conditions that you may have.
Your doctor may ask you to stop taking certain medications such as blood-thinning medications or nonsteroidal anti-inflammatory drugs (NSAIDs), or reduce your use of alcohol or cigarettes.
Ask your doctor whether you need to stop taking any of your medications before the procedure.
Do not eat or drink for at least 8 hours before the procedure. If your doctor has recommended different times, follow the timing recommended by your doctor.
Arrange for someone to drive you home from the hospital.
What can I expect after the procedure?
This procedure usually requires 1 to 2 days of hospital stay, but some people go home the same day as the surgery.
Both mental and physical factors may affect your emotions after a mastectomy. Nurses and other health care professionals are available to talk to you about what to expect and how to deal with your feelings.
It may take you about 6 weeks to fully recover. Ask your doctor when you can expect to return to your usual daily activities.
Following the surgery, dressings and bandages will be applied to the incisions. Stitches and clips used on incisions are usually removed after 7 to 10 days.
The small drainage tubes are usually removed after 1 to 2 weeks, but in some cases they may be removed as early as 1 to 2 days after the procedure.
After this procedure, you will likely feel these normal side effects:
- swelling of the arm or hand: This is caused by a buildup of fluid that flows through the lymph system if the lymph nodes were removed.
- pain or numbness: Pain medications are usually recommended to help control any discomfort. Numbness generally fades with time, but some people experience permanent numbness under the arm if some small nerves were cut.
In addition to this procedure, some women may require other forms of treatment such as radiation, chemotherapy, and hormonal therapy. These additional forms of therapy may be necessary to reduce the risk of cancer recurrence and to improve overall long-term survival.
Upon discharge from the hospital, you should have someone drive you home.
Contact your doctor if you experience the following signs of infection:
- fever
- redness or swelling that worsens
- yellow or green discharge
- foul odour from the incision
Results
Depending on the stage of breast cancer, a successfully performed mastectomy is an effective treatment for breast cancer. The goal of this procedure is to completely remove and prevent recurrence of the breast cancer.
All material copyright MediResource Inc. 1996 – 2024. Terms and conditions of use. The contents herein are for informational purposes only. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Source: www.medbroadcast.com/procedure/getprocedure/Mastectomy