Description of the test
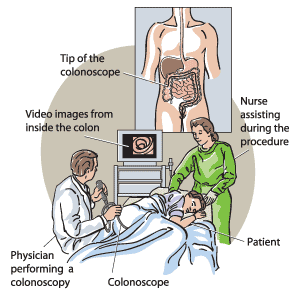
A colonoscopy allows doctors to view the inner lining of the entire colon and rectum. This is the part of your gastrointestinal tract that starts at the bottom of the small intestine and ends at the rectum and anus.
A long, thin, flexible tube with a tiny camera and light, called a colonoscope, is used to conduct this procedure. Looking at a video monitor, your doctor can check for problems such as bleeding, inflammation, or abnormal growths.
How often should the test be performed?
Your doctor will decide when and how frequently this test is required.
Why is this test performed?
A colonoscopy is used to investigate the cause of problems related to the large intestine, such as blood in the stool, constipation, diarrhea, abnormal results of a barium enema test, changes in bowel habits, or anemia.
Colonoscopy is also used as a screening test for colorectal cancer. It is believed that most cases of colorectal cancer start out as polyps. These can be removed during a colonoscopy, before cancer develops. A colonoscopy also allows your doctor to obtain small pieces of tissue (biopsy) for further microscopic examination.
Finally, your doctor can use accessory instruments to perform other tasks, such as obtaining specimens for culture, and treating gastrointestinal bleeding.
Are there any risks and precautions?
Although colonoscopy is generally considered safe, it does have some risk of side effects or complications. Very rare side effects or complications include:
- excessive bleeding at the site of a biopsy or polyp removal. Most bleeding is minor and can be controlled with the colonoscope, or requires no treatment at all.
- a tear through the colon wall, which may need to be repaired with surgery (extremely rare).
- reaction to the sedative (if used)
If you are concerned about any symptoms following this test, speak to your doctor. Take the time to be sure you understand all the risks of complications and side effects as well as any precautions you or your doctor can take to avoid them. Be sure your doctor understands all your concerns.
What happens during the test?
A colonoscopy is usually performed on an outpatient basis at a hospital or clinic. It takes approximately 30 to 45 minutes.
You will need to remove your clothes and wear a gown. You may be given a pain medication and a sedative to help you relax and to relieve some of the discomfort during the procedure, although, if you prefer, it can be done without sedation.
While you are lying on your back or on your left side with your knees drawn up to your chest, your doctor (a gastroenterologist or another qualified health care professional) will gently insert the colonoscope into your rectum and slowly guide it through your colon until it reaches the beginning of the colon or the last section of the small intestines. The flexibility of the instrument allows your doctor to safely navigate the many bends of your colon. In many cases, you may be asked to change position to allow the colonoscope to move along the colon more easily and to provide a better view for the doctor.
The colonoscope will blow air into the colon, inflating it so the doctor can have a better view. The lining of your colon is also examined while the colonoscope is being carefully removed. The camera attached to the end of the colonoscope can also record images that can be studied later.
The test is usually well-tolerated, but during the test you may feel mild cramping, bloating, pressure, an urge to have a bowel movement, and gas pains. Slow and deep breaths may help to lessen this discomfort. You may also occasionally pass gas during the test.
How should I prepare for this test?
Before having this test, discuss the advantages, disadvantages, long-term risks, and consequences associated with the test with your doctor. Be sure you fully understand what will happen and are comfortable with your doctor's answers to your questions.
To perform a colonoscopy safely and effectively, the colon must be empty. Your doctor will give you special instructions on how to do this. In general, you may have to avoid certain foods (such as nuts and seeds) a few days before the colonoscopy. Starting 1 to 2 days before the colonoscopy, you will be required to stop eating solid foods and start a clear liquid diet that does not contain any food colouring but may include:
- coffee or tea (without milk or cream)
- water
- clear broth
- gelatin
- ginger ale
- clear juices
You will be required to use a laxative the night before or possibly the day of the test. The type of laxative prescribed varies. Some laxatives involve taking 4 litres of fluid but if this is not the case, it is important to prevent dehydration by drinking plenty of clear fluids during the diarrhea. In some cases, an enema may be necessary. You may also be asked to stop drinking clear liquids 6 to 8 hours before the test. Read the instructions your doctor gives you carefully and follow the exact instructions provided.
Tell your doctor or prescriber about all prescription, over-the-counter (non-prescription), and herbal medications that you are taking. Also tell them about any medication allergies and medical conditions that you may have.
Also, tell your doctor if you are pregnant or suspect that you might be pregnant.
Ask your doctor or pharmacist whether you need to stop taking any of your medications before the test.
Arrange for someone to drive you home from the hospital.
What can I expect after the test?
You may be asked to stay for observation after the test to allow any medications you have taken to wear off. In addition, you may still feel drowsy and experience cramping and bloating (which is usually relieved by passing gas). You should be able to return to your normal diet after the test, but follow any instruction from your doctor. Drink plenty of liquids to replace the fluids that were lost from using laxatives.
After the test, you should have someone drive you home (or accompany you on public transportation) unless you were not sedated. If you were sedated, you must not drive or operate machinery for the duration advised by your doctor.
If you experience or notice any of the following after the test, contact your doctor immediately:
- dizziness
- fever
- heavy bleeding from the rectum (a small amount of bleeding is normal)
- severe pain and swelling in your abdominal area
- vomiting
Results
The doctor can often discuss the visual results immediately after the test, but may wait until your follow-up appointment. However, if a biopsy was performed, analysis in the lab may take up to a few weeks.
Interpretation of both the visual results and the tissue samples allows the doctor to provide a diagnosis and recommend possible treatments. In some cases, more tests may be necessary.
All material copyright MediResource Inc. 1996 – 2024. Terms and conditions of use. The contents herein are for informational purposes only. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Source: www.medbroadcast.com/procedure/getprocedure/Colonoscopy